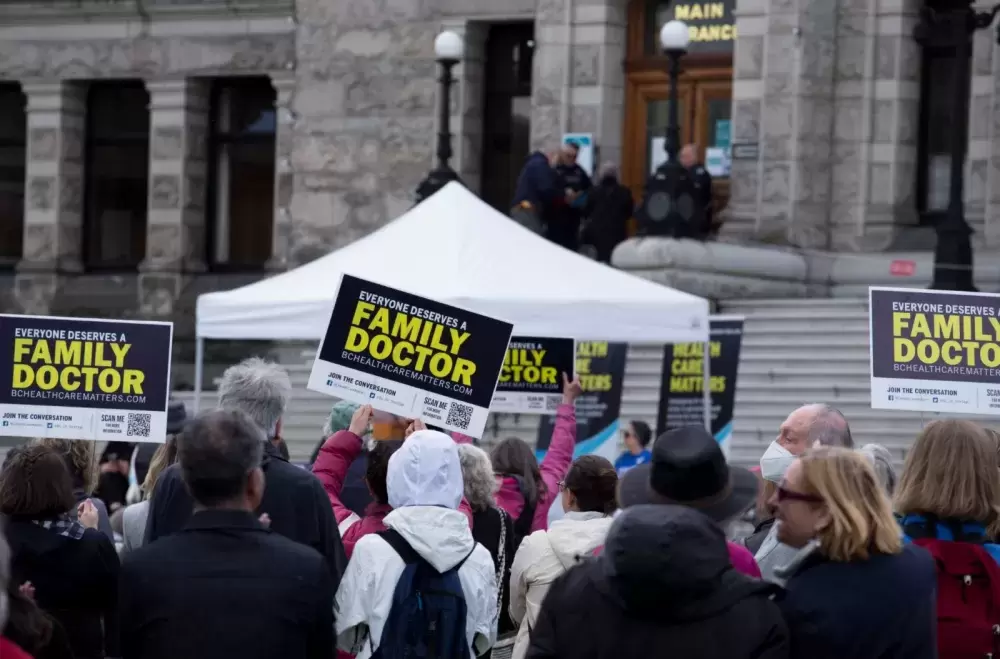British Columbians who have a family doctor can count themselves fortunate, as about 20 per cent of the population - or one in five people - have no regular family physician to go to, according to the BCFamilyDocs website.
The shortage of family physicians is nation-wide problem and is being felt more acutely over the past two years during the pandemic, when COVID-19 cases added pressure to the health care system
But there are other reasons for the doctor shortage, including the fact that there are fewer medical school graduates.
“Fewer medical school graduates are choosing the specialty of family medicine after witnessing the rising expectations placed on family practices without appropriate resources and the resulting physician burnout,” said the College of Family Physicians Canada in a May 2022 statement.
The CFPC has called on the federal government to direct a portion of the announced $3.2 billion investment in recruitment and retention of new health care providers to lighten the administrative load faced by current practitioners.
The provincial government has said that the family physician shortage has been a problem for years and previous governments have made efforts to address it. The current NDP government has committed more than $1 billion to support the sagging health care system. Part of that support is the addition of several hundred new health-care seats in post-secondary institutions.
No one to turn to
How is the doctor shortage affecting Nuu-chah-nulth people living in urban centres?
Ahousaht elder Wally Samuel lives in Port Alberni and requires regular visits to a doctor to stay on top of his health care needs. He was concerned when his family physician announced his retirement. In Port Alberni some family doctors have waiting lists, taking on new patients when they can.
“My doctor had a replacement, which is great,” said Samuel.
He recalled that the replacement doctor spent two weeks in orientation with the senior family doctor, getting to know the patients and their needs.
“Throughout our adulthood we always had access to family doctors,” said Samuel. And doctors that retired always had a replacement.
Samuel is concerned for the people who don’t have family doctors.
“A lot of our people don’t know who to call or where to go,” he noted.
All that is available for those people are walk-in clinics and the emergency department at the hospital. Both places are usually overflowing with patients.
Another related health care issue Samuel pointed out is the difficulty in getting Indian status cards, required for First Nations health coverage.
“There are some kids not yet registered and they have a hard time getting medical,” said Samuel. “I keep telling the politicians that we need better service.”
The situation is different for another Nuu-chah-nulth elder who wishes to remain anonymous. We will call him Elder Two.
Elder Two lives in Nanaimo and is a retired senior citizen. He, his wife and other family members were under the care of a family physician for more than a decade. Elder Two is being treated for diabetes, hypertension, sleep apnea, colon cancer and the aftereffects of a mild stroke. He requires daily prescription medication.
Sadly, their doctor died in July 2022 and the family hasn’t been able to find another family physician.
“He was a good doctor – not being able to find another doctor is very frustrating,” said Elder Two.
He said he’s been getting his required prescriptions by calling online doctor services, but you don’t get the same doctor each time you call. The elder’s damaged blood vessel from his stroke is inoperable and must be treated with medication. But without a family physician, it can be difficult to keep prescriptions up to date.
At one time Elder Two was seen by the physician contracted by the Nanoose First Nation at their Sna-Naw-As Health Care Centre. He was able to get a three-month renewal for his prescriptions. It was good, but it was the only time he would be able to use the service.
“The health care director told me their health care services are only available to their members,” said Elder Two.
A Nuu-chah-nulth woman living in Duncan with her partner has been without a family doctor for three years. We will call her AJ.
Living with a spouse and raising a grandchild, AJ lives on social assistance. She suffers from a medical condition that would qualify her for disability support, but the Ministry of Health requires that the forms be filled out by a family physician.
“The ministry is getting on me, calling me every three months to check and see if I am still on the waiting list,” said AJ.
The small family is living in an RV.
When she has a medical emergency, AJ goes to the Cowichan District Hospital’s emergency department, but says she must wait until it gets “super bad”. AJ went to emergency several times for unexplained abdominal pain and was finally given expensive diagnostic examinations.
“They told me that if I had a family doctor to see, this could have been diagnosed and treated with medication,” she shared. The expensive emergency diagnostic tests could have been avoided.
A revolving door of doctors
Having to be seen in emergency means being treated by a revolving door of doctors. This is true for the phone-in doctor service. While the service is needed and valuable, it doesn’t allow for one single physician to get to know someone’s medical history and offer up suitable treatment plans.
A Nuu-chah-nulth woman living in Port Alberni has relied on the phone-in doctor services for years. We will call her Adult Two.
When Adult Two’s doctor retired, the family did not like the treatment received by the replacement physician. Adult Two says, while the doctor hasn’t said anything overtly discriminatory, he “definitely treats us differently,” she shared.
Adult Two said a family member went into the office seeking information about terminating a pregnancy.
“He gave misinformation about abortion options – told her she had to go to Vancouver for that, but it was too late anyway, then he said he doesn’t kill babies, he brings them into the world,” Adult Two shared.
Adult Two said her relative was left feeling like she had no options at less than five weeks gestation. Adult Two was able to put the relative in contact with suitable health care professionals down island.
When her family needs to see a doctor, they contend with long waits at the hospital emergency department. When her sister’s toddler was sick with a fever, Adult Two offered to drive them to Nanaimo Regional General Hospital’s emergency department, in an effort to avoid long wait times at the West Coast General in Port Alberni.
Adult Two also relies on phone-in doctor services for her own medical needs.
“It’s fantastic, a faster service, but you never get to see the same doctor twice,” she noted.
She appreciates that the phone-in doctors have treated her well and in a professional manner. But when it comes to needing time off work for medical reasons, the doctor’s notes she presents to her employers from the phone-in doctor service are being questioned.
“My employer noticed doctors notes come from different doctors,” said Adult Two.
That’s a problem because it gives the appearance of ‘doctor shopping’. Doctor shopping is a term referring to people that visit many healthcare professionals in an effort to procure multiple prescriptions for medication.
Adult Two says that because of that, she has trouble getting time off work.
“I feel like I’m being discriminated against,” she said.
‘Nobody is taking new patients’
Elder Two said they’ve tried everything possible to get a new doctor, “but nobody, nobody is taking new patients…we have to rely on calling doctor online.”
While he has no regular doctor to check and treat most of his ailments, Elder Two says he regularly sees the doctor that treated his colon cancer.
“I’ve had colon cancer for a long time. I see that doctor every three months to get bloodwork done,” said Elder Two.
Not having a family physician causes Elder Two stress, anxiety and frustration.
“He told me I’m okay and I’m glad he’s still around and keeps me coming to see him,” said Elder Two.
An added concern for Elder Two is his medical records.
“They (former doctor’s office) keep calling me, asking where to send my medical records, but there’s no place to send them. I don’t know what’s going to happen to my records,” he stated.
AJ says she phoned every doctor’s office in Duncan, and nobody is taking new patients, but she managed to get on the waiting list of one.
“I was told people can be on the waiting list for as long as five years before they get picked,” she shared.
The province announced recently that it has invested $118 million in stabilization funding for family doctors. It is working with Doctors of BC on a new physician master agreement and a new compensation model for family physicians.
The funding will also support keeping walk-in clinics open. The province announced that 54 new doctors signed contracts on Oct. 1 to provide full-service primary care in B.C.
In the meantime, elders wait.
“It’s just a matter of plugging away, keep hoping,” said Elder Two.
According to HealthLinkBC, British Columbians may access virtual physicians by calling the 811 Nurses Helpline. From there they will be assessed by a registered nurse and referred to a virtual physician.
In the event of an emergency, such as chest pain, excessive bleeding, difficulty breathing, call 911.